What Is an Ankle Brachial Index Test?
Posted by the medcom group on 23rd Jun 2025
An ankle-brachial index (ABI) test quickly determines if you have peripheral artery disease (PAD). The test is non-invasive, takes just a few minutes, and can confirm a diagnosis for a condition that raises the risk of stroke and heart attack and can lead to limb loss.
Below, we detail how an ankle-brachial index test is performed, how to read the test results, and why it’s an important assessment if your doctor thinks you may have PAD.
What Does an Ankle-Brachial Index Test Check For?
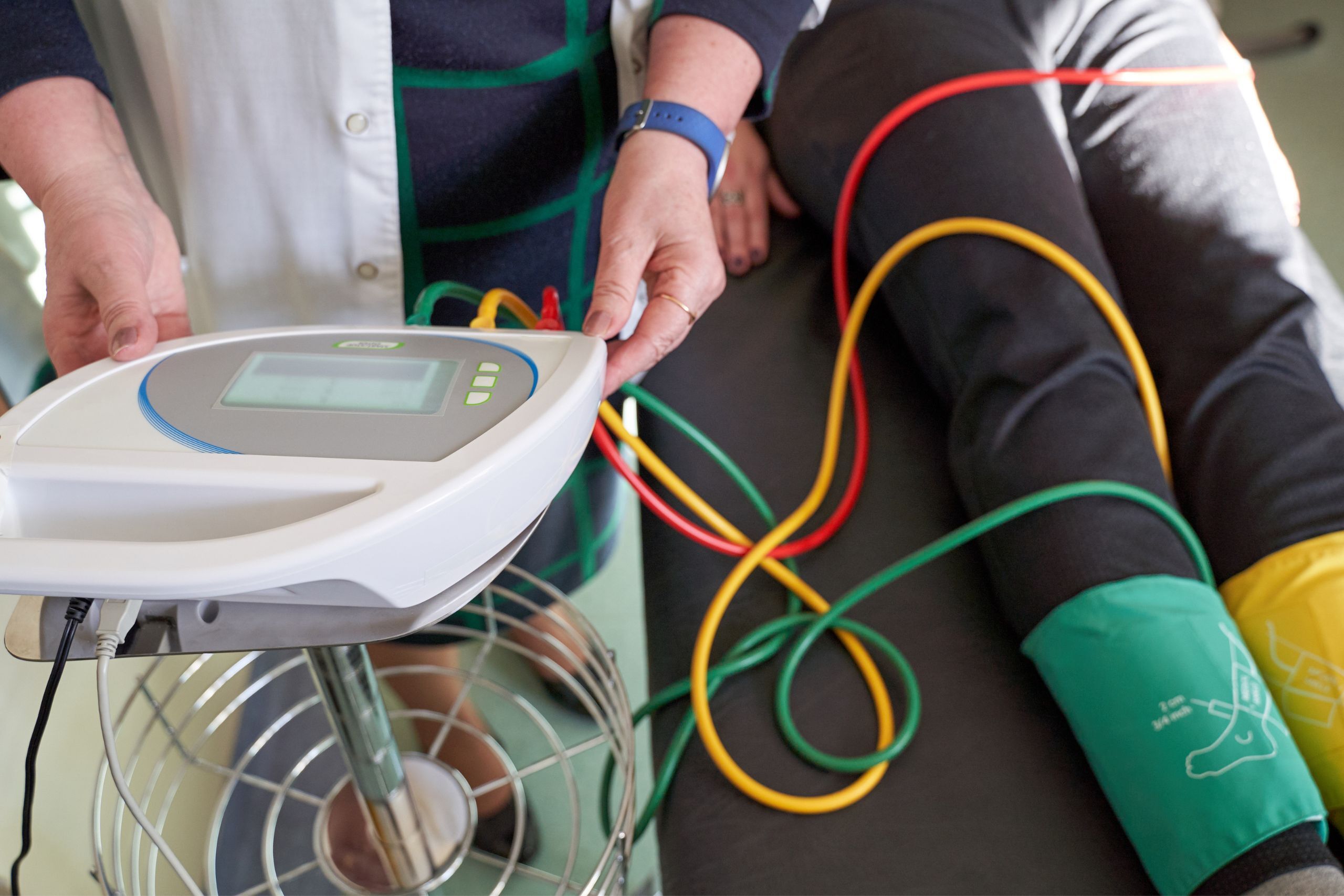
An ankle-brachial index test is used to determine if a patient has peripheral artery disease. PAD is a disease where plaque builds up in the arteries of the legs, buttocks, feet, and (rarely) arms. The narrowed arteries restrict the blood flow to the extremities, which can cause pain and numbness. Other symptoms of PAD can include:
- Muscle pain in the legs that begins with exercise and ends with rest
- Painful cramping in the legs after climbing stairs
- Coldness in the lower foot or leg
- Shiny skin on the legs
- Slow-growing toenails
- Sores on the feet or legs that won’t heal
- Changes in skin color or temperature
While PAD is a fairly common condition, it can have some serious complications. Peripheral artery disease can increase your risk for heart attack and stroke. If left untreated, the narrowed arteries can lead to an appendage not getting sufficient blood flow. When tissue doesn’t get the nutrients it needs from blood, it can start to die. If tissue is damaged beyond repair, doctors may need to amputate a toe, foot, or leg.
If your doctor suspects you may have PAD, they’ll likely order an ankle-brachial index test, the most common and trusted way to test for the disease.
How Is an ABI Test Performed?
An ABI test compares the blood pressure in the upper and lower limbs to see if PAD could be present. It’s a straightforward, pain-free test and takes about 15 minutes to complete.
To perform an ABI test, the medical professional will instruct you to lie down on your back. The clinician will then take your blood pressure in each of your arms. Then, they’ll measure your blood pressure in each of your ankles. They do this by using blood pressure cuffs and a hand-held ultrasound device that's pressed on the skin.
The technician then uses these numbers to compute your ankle-brachial index.
How Do You Read ABI Test Results?
The technician will divide the blood pressure of an ankle by the blood pressure of an arm. This index number will put you into one of the following groups:
- 1.4–1.0: You likely don’t have PAD.
- 1.0–.9: You might have borderline PAD, meaning your peripheral arteries may be starting to narrow, but blood flow through them isn't blocked.
- .9–.7: You likely have mild PAD.
- .7–.4: You likely have moderate PAD.
- Less than .4: You likely have severe PAD.
If you’re experiencing symptoms of PAD but have a high ABI, you may be asked to undergo an exercise ankle-brachial index test. This is a very similar test, but it’s completed before and after you walk on a treadmill, so the medical professional can see how much the arteries are restricted while walking.
Who Should Take an ABI Test?
If you have any symptoms of PAD, your doctor will likely recommend you undergo the easy ankle-brachial index test. Additionally, if you have any of the risk factors for PAD, you may also be a good candidate for the test. Factors that can increase your risk of PAD include:
- Having diabetes
- Smoking
- Being older than 70
- Having plaque formation in other arteries, like in your heart
- Abnormal pulses in your lower legs
- High levels of lipids in your blood
- Being younger than 50 with diabetes and one additional risk factor
What to Do Following a PAD Diagnosis
While an ABI test won’t show exactly which blood vessels are narrowed, it’s an important test for a doctor to know if further treatment is required.
If you are diagnosed with peripheral artery disease or borderline PAD, your doctor will speak with you about treatment options. This may include medications like statins, vasodilators, and blood thinners to open up your arteries and prevent blood clots, which could completely block blood flow and lead to limb removal.
If blood clots are a concern, your doctor may recommend using a sequential compression device (SCD). Also called an intermittent pneumatic compression (IPC) device, these are inflatable sleeves that you slip onto your leg to promote blood flow and prevent clots. SCD machines are used at home while you’re lying in bed or resting in a chair.
If you have PAD or another blood circulation disorder, an SCD can offer peace of mind as you get your treatment protocol dialed in. To learn if an IPC device or a different piece of compression equipment could be a good fit for you, contact our knowledgeable team at the medcom group today.
